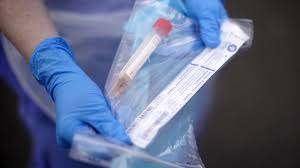
In the early days of the pandemic the wider societal and political concern was the risk that the NHS acute sector would not be able to deal with a massive increase in patients requiring treatment for COVID19. It was at this time that there as a focus on creating capacity within NHS hospitals by ceasing routine non-essential treatments, by maximising the availability of respirators etc. At the same time there was a push to discharge individuals who were fit for discharge either to their own homes or to care homes.
In ordinary circumstances an individual is discharged when they are clinically fit. Before Covid-19 this was often a process which was delayed as a result of the non-availability of care home beds. This was not because the beds were not available but because the funding from public authorities was not sufficient to enable these transfers to take place. Yet even before Covid-19 there were circumstances where at best the eagerness of hospital discharge had led to a breakdown in relationships with the care home sector. The most commonly cited instance was where a clinician considered someone to be able to be supported in residential care, they were then discharged and within hours it was clear they required nursing not residential care. So, looking back from this position we have to be clear that the process of clinical discharge into care homes before Covid19 was one which was not always smooth and frequently problematic. As a result, there was often a local distrust in the system.
This level of challenge was reflected in the Clinical Guidance issued by the Scottish Government on the 13thMarch which stated:
‘Transitions from hospital.
There are situations where long term care facilities have expressed concern about the risk of admissions from a hospital setting. In the early stages where the priority is maximising hospital capacity, steps should be taken to ensure that patients are screened clinically to ensure that people at risk are not transferred inappropriately but also that flows out from acute hospital are not hindered and where appropriate are expedited.’ (page 4)
Because individuals were not routinely tested at the point of discharge at this stage of the pandemic, despite the requests of the care home sector at the time, there was a real concern that people who entered care homes might be infectious.
Scottish Care’s CEO, Dr Donald Macaskill held a meeting on the 18th March with the Cabinet Secretary for Health and Sport and highlighted that care home providers were expressing concern over discharge and that some were refusing to admit new residents. During the meeting he stated that the previous relationships between the acute and care home sector had sometimes not been as good as it might have been. As a positive result of the meeting the Clinical guidance was revised and re-issued on the 26th March.
This Guidance made the process of admission much clearer.
It states:
‘4.2 Admissions/transfer from hospital to care home facilities
HPS updated guidance states that if the individual is deemed clinically well and suitable for discharge from hospital, they can be admitted to the facility after:
- appropriate clinical plan.
- risk assessment of their facility environment and provision of advice about self-
- isolation as appropriate (See NHS Inform for details). (page 4)
- there are arrangements in place to get return them to the facility
Decisions about any follow-up will be on a case by case basis.
If a patient being discharged from hospital is known to have had contact with other COVID-19 cases and is not displaying symptoms, secondary care staff must inform the receiving facility of the exposure and the receiving facility should ensure the exposed individual is isolated for 14 days following exposure to minimise the risk of a subsequent outbreak within the receiving facility.
Individuals being discharged from hospital do not routinely need confirmation of a negative COVID test. Facilities will be advised of recommended infection prevention and control measures on discharge. It is recommended that this includes a documented clinical risk assessment for COVID-19.’ (pages 4-5)
We recognise that from the 21st April it became a requirement for all patients being transferred from hospital to receive a negative test.
Dr Donald Macaskill, the CEO of Scottish Care states:
“It is important to state that amongst those who were Covid positive and who entered care homes in March and April there would be some who were no longer infectious because of the length of stay in hospital. In addition, there would be others who were returning ‘home’ because they could no longer benefit from acute sector care and who were on a palliative and end of life care trajectory. For those individuals it was important that they were able to die in familiar and supportive surroundings. In all cases of knowingly accepting a Covid positive patient as a resident the care home would have instigated robust care and support to ensure the protection of staff and other residents.”